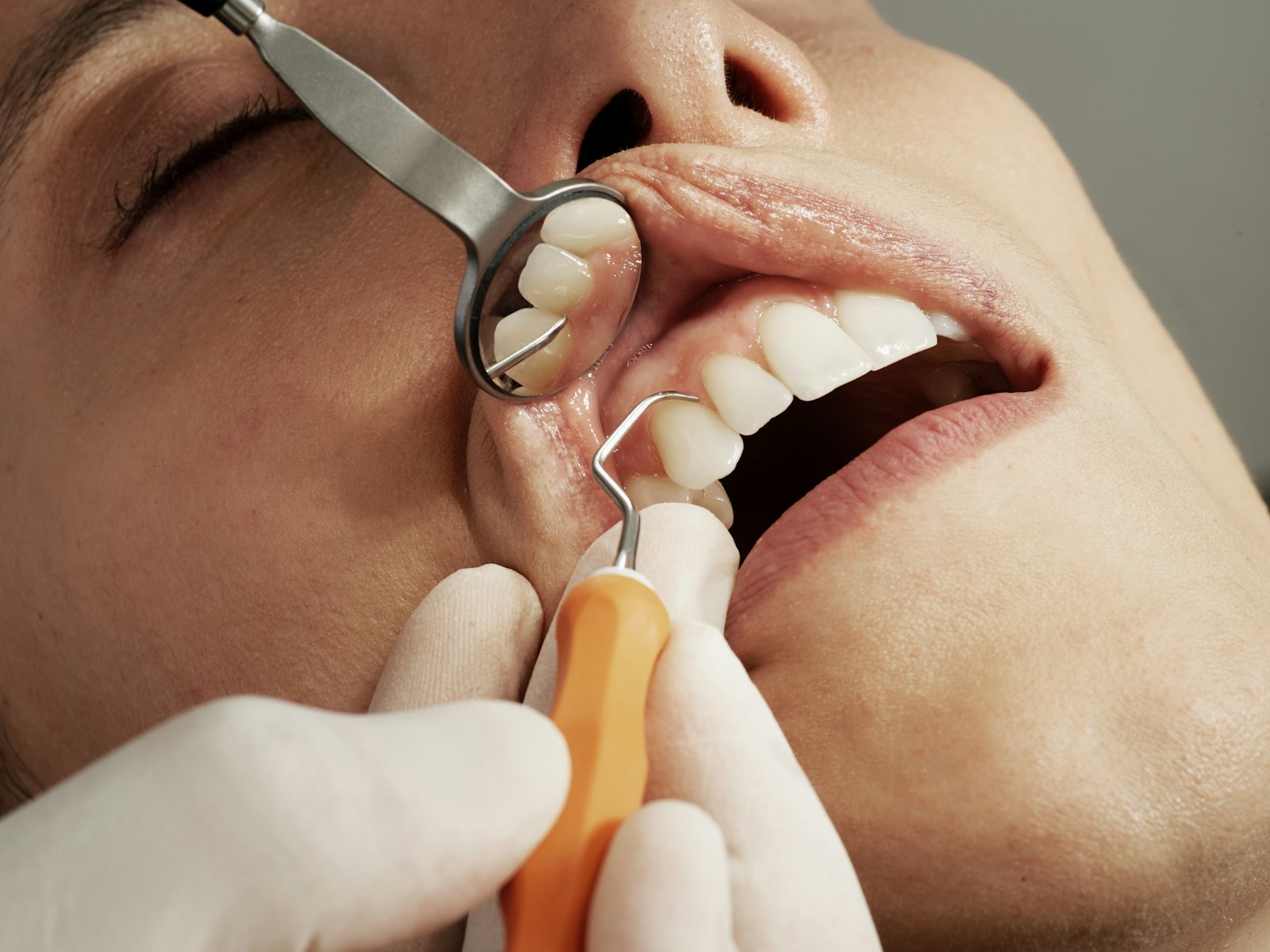
Gum disease is the most common reason adult Australians lose teeth — and the most common reason they don't realise anything is wrong until it has already done damage. About 30% of Australian adults aged 15 and over have moderate to severe periodontitis, the advanced form of gum disease, according to the Australian Institute of Health and Welfare's National Study of Adult Oral Health. The earlier, milder form — gingivitis — affects another 28.8% of adults. Combined, that's well over half the population walking around with some form of active gum inflammation.
The good news: gum disease is highly preventable, the early stage is fully reversible, and even advanced cases can usually be stabilised with the right treatment. This Sydney guide explains the stages, what causes it, the warning signs, what treatment looks like at each stage, and what it typically costs.
Key takeaways
- Gum disease has two main stages. Gingivitis (early, fully reversible) and periodontitis (advanced, manageable but not reversible). Around 1 in 3 Australian adults has moderate to severe periodontitis.
- Bleeding gums when you brush or floss is the earliest warning sign — and the one most people ignore. Healthy gums do not bleed.
- Treatment costs in Sydney typically range from $135 for a standard scale and clean (gingivitis) to $1,000–$3,000 for active periodontal therapy across multiple visits. Severe cases requiring surgery can exceed $5,000.
- Periodontitis is permanent — but stoppable. Lost bone and gum tissue does not grow back, but proper treatment can halt progression and prevent tooth loss.
- Smokers are 3–6 times more likely to develop severe periodontitis and respond more slowly to treatment, according to the Australian Dental Association.

What is gum disease?
Gum disease (periodontal disease) is a chronic inflammatory infection of the tissues that hold your teeth in place — the gums, the periodontal ligament, and the underlying jaw bone. It starts when plaque, a soft sticky film of bacteria, is left on the teeth long enough to harden into tartar (calculus) along the gumline. Your immune system reacts to the bacteria, the gums become inflamed, and over time the inflammation spreads downward and outward — eventually destroying the bone that anchors the teeth.
The progression is silent. Most people feel no pain until the disease is well advanced, which is why routine dental check-ups matter even when nothing seems wrong. The dentist or hygienist measures the depth of the small space between gum and tooth (the "pocket") with a thin probe — healthy pockets are 1–3 mm; pockets of 4 mm or more suggest active disease.
The stages of gum disease
Modern classification, adopted in Australia after the 2018 World Workshop on Periodontology, splits gum disease into gingivitis and four stages of periodontitis. Knowing which stage you're in determines what treatment looks like and how predictable the outcome is.
Stage 1: Gingivitis (fully reversible)
The earliest and only fully reversible stage. Gums are red, slightly swollen, and bleed when you brush or floss. There is no bone loss yet — only inflammation of the gum tissue. With a professional clean and a couple of weeks of consistent home care, gingivitis disappears completely. If left alone, however, around 10–15% of cases progress to periodontitis.
Stage 2: Stage I periodontitis (mild)
Pockets of up to 4 mm, mild bone loss visible on X-rays (typically less than 15% of the tooth's supporting bone), and no teeth lost yet. Still highly treatable with non-surgical care. Most patients at this stage report nothing more than occasional bleeding when flossing.
Stage 3: Stage II periodontitis (moderate)
Pockets of up to 5 mm, moderate horizontal bone loss (15–33%), and gum recession that the patient may now be able to see in the mirror. Non-surgical deep cleaning is the usual first step; some patients also need surgical treatment to access deeper pockets. Teeth are still firm.
Stage 4: Stage III periodontitis (severe)
Pockets of 6 mm or more, vertical bone loss, possibly furcation involvement (bone loss between the roots of multi-rooted teeth), and the potential loss of up to 4 teeth. Surgical periodontal treatment, sometimes combined with regenerative grafting, is usually required.
Stage 5: Stage IV periodontitis (advanced)
The most severe stage. Multiple teeth are loose, drifting, or already lost, and the patient's bite is affected. Treatment becomes complex — periodontal therapy is combined with prosthodontics (crowns, bridges, implants, or dentures) to restore function. Care is usually shared between a periodontist and a general dentist.
What causes gum disease?
Plaque is the trigger, but several factors decide who progresses from healthy gums to gingivitis to periodontitis — and how fast.
1. Inadequate plaque control
The single biggest factor. Plaque that sits on the teeth for more than 24–48 hours starts to mineralise into tartar, which can no longer be brushed away and shelters more bacteria underneath. Most people brush adequately but skip flossing or interdental brushes, which is where most early disease starts.
2. Smoking and vaping
Smokers are 3–6 times more likely to develop severe periodontitis than non-smokers, and they often have less obvious bleeding (nicotine constricts blood vessels), which masks the warning signs. The 2018 ADA review concluded smoking is the strongest modifiable risk factor for periodontitis. Vaping carries similar risks based on emerging evidence.
3. Diabetes
Poorly controlled diabetes and gum disease have a two-way relationship: diabetes makes you more susceptible to gum infections, and gum disease makes blood-glucose harder to control. Patients with HbA1c above 7% are at meaningfully higher periodontal risk.
4. Genetics
Some people have an inherited inflammatory response that makes them more vulnerable. If a parent had severe gum disease or lost teeth to it, your risk is higher even with good home care — meaning more frequent maintenance visits.
5. Hormonal changes
Pregnancy, the contraceptive pill, and menopause can all amplify the gum's inflammatory response to plaque. "Pregnancy gingivitis" affects up to 75% of pregnant women in some studies — usually peaking in the second trimester and resolving after birth.
6. Stress
Chronic stress raises cortisol, which suppresses the immune response and shifts oral bacteria toward more pathogenic species. Acute necrotising gingivitis — a rare painful form sometimes called "trench mouth" — is closely linked to extreme stress and exhaustion.
7. Medications
Some blood pressure medications (calcium-channel blockers like amlodipine), anti-seizure medications (phenytoin), and immunosuppressants (cyclosporin) can cause gum overgrowth that traps plaque. Many other medications cause dry mouth, which raises plaque bacteria counts.
8. Crowded or crooked teeth
Teeth that overlap, tilt, or have deep grooves create areas a toothbrush can't reach. People with significant crowding often have more localised gum disease around the hardest-to-clean teeth, even with otherwise excellent home care.

Signs and symptoms to watch for
Most people with early gum disease feel completely normal. The signs that something is wrong are visual and tactile — and easy to overlook unless you know what to look for. See a dentist if you notice any of the following:
- Bleeding when you brush or floss — even a small amount of pink in the spit. Healthy gums do not bleed at all.
- Gums that look red, puffy, or shiny at the edge instead of pale pink and stippled.
- Persistent bad breath or a bad taste that doesn't improve with brushing — often the first thing a partner notices.
- Receding gums or teeth that look longer than they used to. (For more on this specific sign, see our receding gums guide.)
- Sensitivity to cold or sweet, particularly along the gumline where root surface has been exposed.
- A change in how your teeth fit together when you bite down, or teeth that feel slightly loose.
- Pus around a tooth, dull throbbing, or a tender swelling — these point to an active periodontal abscess and warrant a same-day appointment.
How dentists diagnose gum disease
Diagnosis is straightforward and painless. A typical periodontal assessment takes 15–25 minutes and includes:
- Periodontal probing. A thin marked probe gently measures the pocket depth at six points around every tooth. Depths of 1–3 mm are healthy; 4 mm or more suggests active disease.
- Bleeding on probing. The probe also reveals which sites bleed, indicating inflammation.
- Radiographs. Bitewing or periapical X-rays show how much supporting bone has been lost, which is what distinguishes gingivitis from periodontitis.
- Recession measurement. The amount of root surface exposed where the gum has shrunk away.
- Mobility check. A gentle test of whether each tooth moves under finger pressure.
The dentist combines these findings into a stage (I–IV) and a grade (A, B, or C — based on the rate of progression). The stage determines what treatment is needed; the grade determines how aggressive the maintenance plan should be.
Gum disease treatment options and Sydney costs
Treatment is matched to the stage. Mild cases often respond to a single thorough clean; advanced cases may need months of staged care. The table below shows typical Sydney private-fee ranges (no insurance applied) drawn from the 2025 Australian Dental Association Schedule and Sydney clinic surveys. Item codes refer to the ADA Australian Schedule of Dental Services.
| Treatment | ADA item | Typical Sydney cost | When it's used |
|---|---|---|---|
| Comprehensive exam + X-rays | 011, 022, 037 | $220–$380 | First-visit baseline assessment |
| Standard scale and clean | 114, 121 | $135–$280 | Gingivitis or maintenance |
| Periodontal debridement (whole mouth) | 213, 214 | $250–$500 | Heavy tartar load before deep cleaning |
| Root planing per quadrant (deep clean) | 222 × 4 quadrants | $200–$350 per quadrant | Stage I–II periodontitis |
| Active periodontal therapy (full course) | multi-visit | $1,000–$3,000 | Stage II–III periodontitis |
| Periodontal flap surgery (per quadrant) | 241 | $700–$1,400 | Stage III periodontitis with deep pockets |
| Guided tissue regeneration / bone graft | 245, 246 | $1,500–$3,500 | Stage III–IV with vertical bone loss |
| Gum graft (free gingival or connective tissue) | 252, 253 | $1,800–$3,500 | Significant recession around individual teeth |
| Specialist periodontist consultation | 014, 022 | $300–$450 | Severe or rapidly progressing disease |
| Supportive periodontal therapy (per visit, every 3 months) | 222 | $200–$350 | Lifelong maintenance after active treatment |
Most private health funds offer some periodontal cover under "major dental" or "general dental" depending on your level — usually with annual limits of $700–$1,500. Medicare covers eligible children under the Child Dental Benefits Schedule and adults under specific public dental schemes; routine adult periodontal care is otherwise not covered.
Can gum disease be reversed?
Gingivitis can be fully reversed. A professional clean to remove tartar plus 10–14 days of consistent brushing and flossing returns the gums to health, with no permanent damage left behind.
Periodontitis cannot be reversed — but it can be stopped. Once bone has been lost, it does not regenerate on its own. Even with surgical regenerative grafts, only a portion of lost bone can be rebuilt. The realistic goal of periodontal treatment is to halt progression: stabilise the pockets, eliminate inflammation, and prevent further bone loss. Done well, this preserves the teeth indefinitely.
This is why early diagnosis matters so much. Gingivitis treated promptly costs a single scale and clean. Periodontitis treated late costs many thousands of dollars and risks tooth loss anyway.
How to prevent gum disease (start tonight)
The home-care routine that prevents gum disease is the same one that treats early gingivitis. None of it is glamorous — it is consistency that does the work.
- Brush twice a day for two minutes with a soft-bristle brush angled 45° toward the gumline, using small circular motions (the modified Bass technique). An electric brush with a pressure sensor reduces the effect of brushing too hard.
- Clean between every tooth, every day. Floss, interdental brushes, or a water flosser — whichever one you will actually use. About a third of the tooth surface is between teeth and a brush cannot reach there.
- Use a fluoride toothpaste. Look for at least 1,000 ppm fluoride. Most major-brand pastes meet this; some "natural" pastes do not.
- Replace your brush every 3 months — or sooner if the bristles splay. A frayed brush cleans poorly.
- See a dentist every 6 months for a check-up and clean. If you've already had periodontitis, the recall interval drops to 3 months for life.
- Stop smoking and limit alcohol. Smoking is the single biggest controllable risk factor; quitting at any age improves your gum response to treatment within 6–12 months.
- Manage the underlying conditions. Keeping diabetes, stress, and hormonal fluctuations under control directly improves gum-tissue resilience.
Other habits worth getting right: brush before bed (overnight saliva flow drops, so plaque builds faster), don't rinse with water after brushing (it washes the fluoride away — just spit), and consider an alcohol-free antibacterial mouthwash if you're prone to gingivitis. If you're already noticing persistent bad breath or sensitive teeth along the gumline, those can be early warning signs that home care alone may not be enough.
Frequently asked questions
How do I know if I have gum disease?
The earliest and most reliable sign is bleeding when you brush or floss. Healthy gums do not bleed. Other clues are persistently bad breath, gums that look red rather than pale pink, sensitivity along the gumline, and any feeling that a tooth has shifted or feels loose. The only way to confirm and stage the disease is a dental examination with periodontal probing and X-rays.
Is gum disease painful?
Usually not until it's advanced. Both gingivitis and early periodontitis are typically painless — which is why most people don't seek treatment until significant damage has already occurred. Pain, swelling, or pus suggests a periodontal abscess, which needs same-day care.
Can I treat gum disease at home?
Gingivitis can often be reversed at home with rigorous brushing and flossing for 10–14 days, but only if you have already had a professional clean to remove the hardened tartar. Once tartar is present, no amount of brushing will remove it — it has to be scaled off. Periodontitis always needs professional treatment; home care alone cannot stop it.
Does my health fund cover gum disease treatment?
Most private health funds with general or major dental cover include some periodontal benefits — typically a percentage rebate on scaling, root planing, and periodontal surgery, subject to your annual limit. The rebate amount and waiting periods vary widely between funds. Call your insurer with the ADA item codes (e.g. 222, 241, 245) for a per-procedure quote before booking.
How long does gum disease treatment take?
Gingivitis often resolves within 2–3 weeks of a single scale and clean. Active periodontal therapy for moderate to severe periodontitis usually involves 4–6 visits over 2–3 months, followed by re-evaluation at 3 months, then ongoing maintenance every 3 months for life. Surgery, where needed, adds 4–6 weeks of healing.
Will I lose my teeth?
Not necessarily — and not if treatment starts early. Stage I and II periodontitis treated promptly preserves all teeth in the vast majority of cases. Stage III may involve losing 1–4 teeth that have been too compromised to save. Stage IV usually involves replacing several missing teeth with bridges, dentures, or implants. Smokers, uncontrolled diabetics, and patients who skip maintenance visits have substantially higher tooth-loss rates.
Can stress really cause gum disease?
Stress alone doesn't cause gum disease, but it makes plaque-driven inflammation worse. Chronic stress raises cortisol, suppresses the immune response, and is strongly linked to bruxism (teeth grinding) — all of which compound periodontal damage. If anxiety is part of the picture, our dental anxiety guide explains how Sydney clinics can help you keep up with maintenance visits without dread.
The bottom line
Gum disease is the most common reason adult Australians lose teeth — and almost always preventable when caught early. Bleeding when you brush is not normal. The earlier the diagnosis, the simpler and cheaper the fix: a $135 scale and clean for gingivitis, against many thousands and the risk of tooth loss for late-stage periodontitis. Even severe cases can be stabilised with the right care.
If it has been a while since your last dental cleaning, or you've been quietly hoping the bleeding will sort itself out, it won't — but a single visit will tell you exactly where you stand and what (if anything) needs to be done. Lumi Dental in Melrose Park, Sydney, is opening 1 July 2026 with comprehensive periodontal assessments and gentle hygiene-led care for new and returning patients.