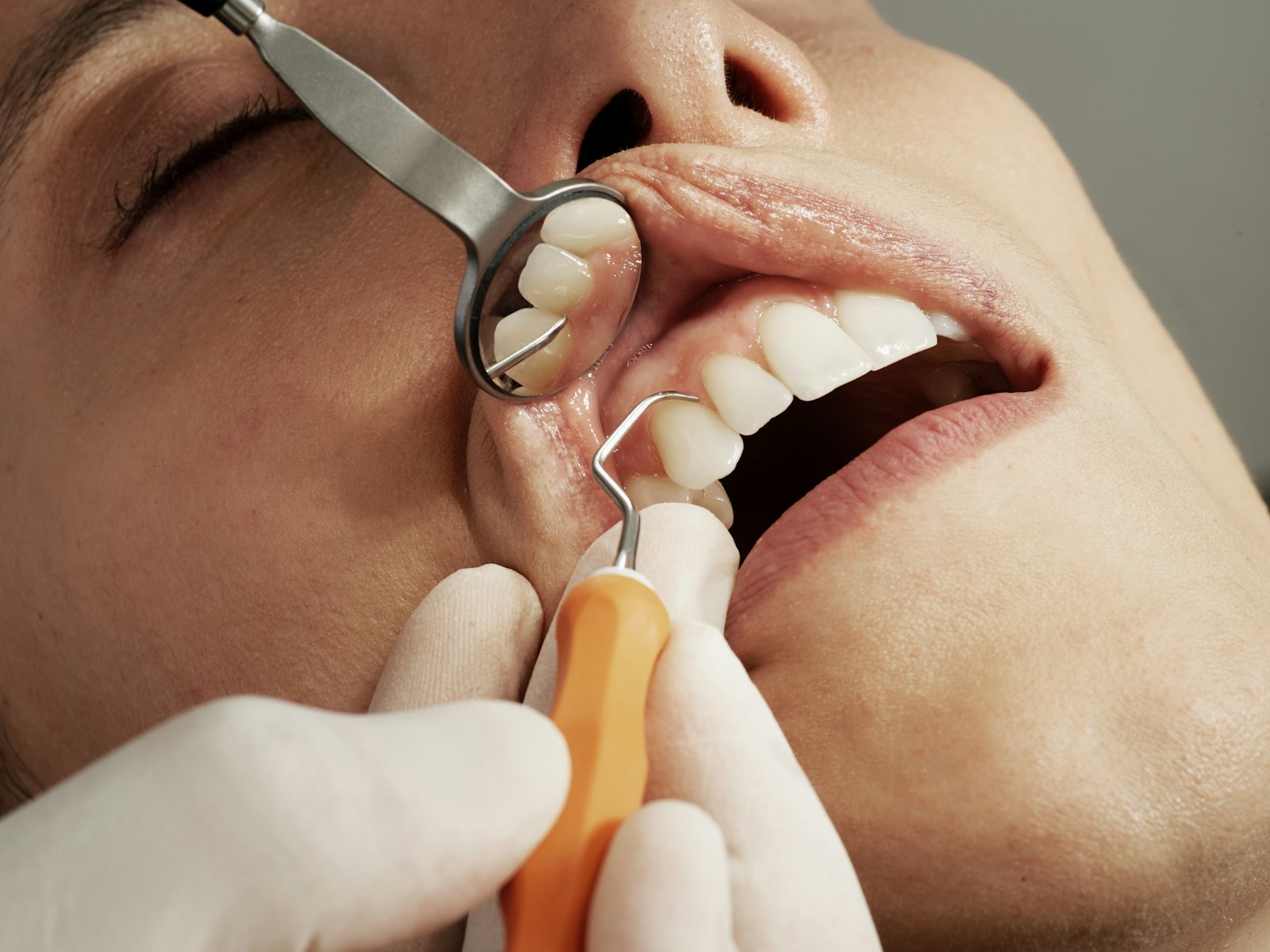
If you wake up with a sore jaw, a dull headache around your temples, or your partner has mentioned a grinding sound at night, you may be one of the many Australians living with bruxism without realising it. Most people who grind their teeth are not aware they are doing it, and the damage tends to build up quietly over months and years before something forces the issue: a cracked back tooth, a filling that keeps failing, or a partner who finally raises it.
This guide explains what bruxism actually is, how to tell if you have it, why it happens, the full range of treatment options, and what each of them costs in Sydney.
Key takeaways
- Bruxism is the involuntary grinding or clenching of teeth, most often during sleep, affecting an estimated 8 to 16 percent of adults globally according to the 2024 systematic review in the Journal of Clinical Medicine.
- It is not a habit you can simply stop. Sleep bruxism is now classified as a sleep-related movement behaviour, with stress, sleep-disordered breathing, certain medications and lifestyle factors all contributing.
- The damage shows up as flattened front teeth, cracked back teeth, sore jaw muscles, morning headaches, gum recession and worn-through fillings.
- Treatment combines a properly fitted occlusal splint, addressing the underlying drivers (stress, sleep, lifestyle), and restoring damaged teeth where needed. A splint protects, but it does not cure the cause.
- Sydney costs range from $20 for a chemist boil-and-bite mouthguard up to $9,000 or more for full-mouth restorative work after years of untreated grinding.
What bruxism actually is
Bruxism is the involuntary grinding, clenching or gnashing of the teeth. The dental and sleep medicine communities now split it into two distinct conditions, because they have different causes and different treatments.
Sleep bruxism
Sleep bruxism happens during sleep and is classified by the American Academy of Sleep Medicine as a sleep-related movement disorder. It is rhythmic, often loud enough for a partner to hear, and produces forces several times higher than awake clenching because the normal protective reflexes that keep teeth apart during the day are reduced. People with sleep bruxism are not consciously controlling it and cannot simply stop.
Awake bruxism
Awake bruxism is a clenching habit, usually during concentration, driving, screen time or stress. It is more common in women and is often part of a broader pattern of muscle tension that includes shoulders, neck and jaw. Unlike sleep bruxism, awake bruxism responds well to habit awareness training because the patient can learn to notice and release the clench.
Why the distinction matters
Most people have one form or the other, but a meaningful minority have both. The distinction matters because a splint is the standard treatment for sleep bruxism but not for awake bruxism, where the gains come from habit retraining and stress management. Confusing the two is one of the most common reasons treatment underperforms.
How common is bruxism in Australian adults?
The 2024 systematic review and meta-analysis in the Journal of Clinical Medicine pooled data from 99 studies and reported a global sleep bruxism prevalence of 21 percent and awake bruxism prevalence of 23 percent across the general population. For adults specifically, the range is narrower, between 8 and 16 percent for sleep bruxism, depending on whether the diagnosis is self-reported, partner-reported or confirmed with sleep recording.
Australia-specific population data is limited, but the Australian Institute of Health and Welfare's National Study of Adult Oral Health flagged tooth wear as a growing concern, with around 1 in 4 Australian adults showing visible enamel wear by age 35. Bruxism is the leading non-dietary cause of that wear pattern.
What this means in practice: in a typical Sydney suburb of 10,000 adults, somewhere between 800 and 1,600 people are grinding their teeth at night, and most of them have no idea.
Signs and symptoms to watch for
Bruxism is usually picked up by one of three routes: a partner hears the grinding, the person notices a pattern of morning symptoms, or a dentist spots the wear at a routine examination. The symptoms below frequently overlap, and having two or three of them is a stronger signal than any one alone.
1. Morning jaw stiffness or muscle fatigue
The masseter muscles on the sides of the jaw and the temporalis muscles at the temples can be sore, tight or fatigued on waking. The pain typically eases through the morning as the muscles loosen, which is the opposite pattern to most other dental pain.
2. Headaches that fade as the day goes on
A dull pressure-type headache around the temples or forehead, present on waking and easing within a few hours, is classic for nocturnal clenching. It is often misattributed to dehydration, screen time or sinus pressure.
3. Flattened, chipped or worn front teeth
The canines and incisors lose their natural pointed contour and become flat across the biting edge. Small chips appear on the corners. The back teeth may show shiny worn facets where the upper and lower teeth meet.
4. Cracked teeth or repeatedly failing fillings
A history of more than one cracked tooth, or fillings and crowns that keep coming loose or breaking, is a strong indicator that the bite is taking more force than the tooth structure can handle.
5. Increased tooth sensitivity
As enamel wears thin, exposed dentine triggers cold and pressure sensitivity. Patients often try desensitising toothpaste for months without realising bruxism is the underlying driver.
6. Jaw clicking, popping or limited opening
Sustained muscle overload places strain on the temporomandibular joint. A clicking sound on opening, tenderness at the joint, or difficulty opening wide first thing in the morning all suggest the joint is being affected.
7. Indentations on the tongue or a ridge along the cheek
A scalloped tongue edge or a horizontal white ridge along the inside of the cheek (the linea alba) shows that teeth are pressing into soft tissue during the night. These are silent signs the patient never notices but a dentist will see immediately.
8. Audible grinding heard by a partner
The most reliable single sign. If someone has told you they hear grinding, believe them. The forces during sleep grinding can be loud enough to wake a partner in a quiet room.

Why bruxism happens: the six main drivers
Bruxism rarely has a single cause. The current evidence points to a cluster of contributing factors that vary in importance from person to person.
1. Stress and anxiety
Psychological stress is the most consistently identified driver. Sympathetic nervous system activation increases muscle tone, and clenching becomes a learned response to tension. Periods of work pressure, relationship stress or grief frequently coincide with the first noticeable symptoms.
2. Sleep-disordered breathing
Sleep bruxism shares a strong association with obstructive sleep apnoea and snoring. The current model is that micro-arousals from breathing disruption trigger masticatory muscle activity. In some patients, treating the airway reduces grinding without any dental treatment. This is why a thorough assessment asks about snoring, witnessed pauses in breathing and daytime tiredness.
3. Stimulants, alcohol and certain medications
Caffeine after midday, alcohol within three hours of sleep, nicotine and recreational stimulants all increase sleep bruxism episodes. SSRIs, some ADHD medications and certain antipsychotics are documented triggers. This does not mean stopping your medication, but it is worth discussing with the prescribing doctor if grinding has worsened since starting something new.
4. Bite and dental factors
The role of malocclusion in bruxism has been overstated historically. Minor bite irregularities are not a primary cause, but a missing back tooth, a high filling or a poorly contoured crown can worsen existing tendencies.
5. Genetics and personality factors
People who report a parent or sibling with grinding are more likely to grind themselves. Personality traits associated with bruxism include high competitiveness, perfectionism and a tendency to suppress rather than express tension.
6. Children and adolescents: a special case
Up to 30 percent of children grind their teeth at some point, with the highest rates between ages 3 and 6. Most outgrow it as the adult dentition erupts. Persistent grinding into adolescence with worn primary teeth or daytime fatigue warrants assessment.
The hidden cost: what untreated bruxism does to teeth
Forces during sleep grinding can reach 5 to 10 times normal chewing pressure. Over years, this load drives a predictable cascade of damage.
Year one to three: microscopic enamel wear, mild morning muscle fatigue, occasional cold sensitivity.
Year three to seven: visible flattening of front teeth, first chips on incisal edges, increased sensitivity, recurrent jaw muscle tension, first failed restorations.
Year seven and beyond: structural cracks in molars (often presenting as cracked tooth syndrome), loss of vertical face height, gum recession at the canines and premolars from abfraction lesions, pulp damage requiring root canal treatment, and crowns or onlays needed to rebuild lost tooth structure.
The financial scale is substantial. A patient who arrives at age 50 having ground unmanaged for 20 years frequently needs $8,000 to $25,000 of restorative work to rebuild what wear has taken. The same patient, treated at age 35 with a $700 splint, would have been protected for far less.
How bruxism is diagnosed
There is no single test for bruxism. Diagnosis combines clinical examination, history and, in selected cases, sleep studies.
Clinical examination
The dentist maps tooth wear, palpates the masseter and temporalis muscles for tenderness, checks the jaw joint for clicking, measures opening range, and inspects the tongue and cheeks for soft tissue signs. Photographs and intraoral scans document the current state so progression can be tracked.
History
Questions cover sleep quality, snoring, witnessed apnoeas, daytime fatigue, headache pattern, stress level, caffeine and alcohol intake, current medications and family history. Partner-reported grinding is one of the strongest single pieces of evidence.
Sleep recording (when needed)
For patients with suspected sleep apnoea, daytime sleepiness, or grinding that has not responded to splint therapy, an at-home sleep study or laboratory polysomnography can confirm sleep bruxism and identify any breathing disorder. This is arranged through a sleep physician.
Wearable EMG monitors
At-home devices using surface electromyography count clenching events overnight. They are useful for awake bruxism habit retraining and for measuring response to treatment, but are not a primary diagnostic tool.
Treatment options and what each costs in Sydney
The treatment plan depends on the severity, the dominant driver (stress, sleep, lifestyle, dental) and the amount of damage already present. Most patients need a combination, not a single intervention. The following table summarises the main options and typical Sydney fee ranges, with ADA item codes where applicable. Costs vary by individual case, splint design and any health fund rebates. This is general information, not a quote.
| Treatment | ADA item | Typical Sydney range | Best suited for |
|---|---|---|---|
| Comprehensive examination, photographs, X-rays | 012/013/022/037 | $80–$350 | All new patients, before any treatment |
| Boil-and-bite chemist mouthguard | n/a | $20–$60 | Short-term protection while waiting for assessment |
| Soft or dual-laminate night guard (lab-made) | 963 | $300–$650 | Mild grinders, athletes returning to sport |
| Custom hard occlusal splint (lab-made) | 963 | $400–$900 | Moderate to heavy grinders, jaw joint symptoms |
| Anterior deprogramming splint (e.g. NTI) | 963 | $500–$900 | Selected cases under specialist supervision |
| Botulinum toxin to masseter muscles | n/a (medical) | $400–$700 per session, every 3–6 months | Severe muscle hypertrophy, refractory cases |
| Physiotherapy for TMJ and masticatory muscles | n/a (allied health) | $95–$160 per session | Persistent muscle pain, jaw joint involvement |
| Cognitive behavioural therapy or biofeedback | n/a (psychology) | $180–$250 per session | Stress-driven and awake bruxism |
| Sleep study referral and CPAP if indicated | n/a (medical) | Bulk-billed to $300 study; CPAP $1,200–$2,500 | Suspected sleep-disordered breathing |
| Restorative repair of worn or cracked teeth (composite, onlay, crown) | 521–615 | $220–$2,500 per tooth | Patients with established damage |
| Full-mouth rehabilitation for advanced wear | various | $15,000–$60,000+ | Severe long-standing cases with collapsed bite |
Most private health funds with general or major extras rebate part of the splint fee under item 963. Rebates typically range from $100 to $300 depending on the fund, policy and remaining annual cap. Botulinum toxin and psychology sessions may attract Medicare rebates under specific care plans arranged through your GP.
Splints in detail: which type for which patient
The terminology around splints is genuinely confusing because the same word means different things to different people. A clearer framework:
Sports mouthguard
Soft, shock-absorbing, designed for contact sport. Not suitable as a night guard because the soft material encourages chewing rather than discouraging it.
Boil-and-bite chemist guard
Softens in hot water and moulds to your teeth. Reasonable as a short-term bridge while waiting for a custom appliance, but bulky, fast-wearing and prone to causing bite changes if worn for months.
Soft or dual-laminate night guard
A laboratory-made appliance with a soft inner layer and harder outer surface. Well-tolerated and cheaper than a hard splint, but less protective for heavy grinders because the soft surface compresses under load.
Hard acrylic occlusal splint
The standard option for moderate to heavy bruxism. Made from a digital scan or impression and adjusted on your bite at fit. Distributes biting forces evenly, allows the jaw muscles to settle, and protects enamel and existing restorations. Expected lifespan three to five years.
Anterior deprogramming splint
A small splint covering only the front teeth, designed to prevent the back teeth from contacting at night. Effective in selected cases for breaking heavy clenching cycles, used cautiously and short term because of the risk of back-tooth movement if worn long term without supervision.
What an assessment looks like
A first appointment for suspected bruxism is diagnostic, not a rush to make a splint. A typical 45 to 60 minute new-patient visit covers:
- History. Sleep, stress, partner-reported grinding, headache pattern, medications, caffeine and alcohol intake, family history.
- Examination. Tooth wear mapping, restoration assessment, jaw muscle palpation, joint check, opening range, soft tissue review.
- Imaging. Standard X-rays where indicated, plus intraoral photographs and a digital scan to document the current state.
- Discussion. What the wear pattern shows, which drivers are likely contributing, what the options are, what each one costs.
- Plan. Often a splint plus one or two lifestyle adjustments. Sometimes a referral to your GP for sleep assessment. Occasionally just monitoring with annual photographs if the wear is mild and stable.
If a splint is appropriate, the next visit is for the digital scan. The lab takes about two weeks. A fit appointment follows, with a short adjustment to the bite, and a review at four to six weeks checks how you are sleeping with it.
What you can do tonight, before you see anyone
If you are reading this with a sore jaw and waiting for an appointment, the following are reasonable steps that are unlikely to make things worse.
- Cut caffeine after midday for the next two weeks: coffee, energy drinks, dark chocolate, some teas.
- Move alcohol earlier. Finish wine or spirits at least three hours before sleep. Alcohol fragments sleep and increases grinding episodes.
- Apply a warm compress to the jaw before bed for 10 minutes to loosen the masseter muscle.
- Practise jaw release. Place the tongue gently on the roof of the mouth behind the front teeth. The teeth should naturally separate by a few millimetres. Notice this position whenever you catch yourself clenching during the day.
- Avoid chewy foods. Steak, hard bread, chewing gum and tough lollies fatigue an already overworked muscle. Soft food for a week often settles soreness substantially.
- Simple analgesia if needed. Paracetamol 1 gram up to four times a day, or ibuprofen 400 milligrams up to three times a day with food, for short-term muscle pain. Check with a pharmacist if you take other medications.
- Chemist boil-and-bite guard for a few nights if you have ongoing damage. Not a long-term solution, but better than nothing while you wait.
This is not a treatment plan. It is what to do while you organise an appointment.
Preventing the next stage of damage
Prevention sits on three pillars.
Protect
A well-fitted splint worn consistently every night. Patients who skip nights when travelling or after a few drinks often see wear continue at half speed rather than stop. Consistency matters more than splint design.
Address the driver
Identify which of the six drivers applies to you and act on it. Stress-driven cases benefit from cognitive behavioural therapy, mindfulness practice or a workload conversation. Sleep-driven cases need a GP review and possibly a sleep study. Lifestyle cases respond to the caffeine and alcohol changes above. The splint protects the teeth, but only addressing the cause reduces the muscle activity itself.
Restore early, not late
Worn enamel does not regenerate, and cracks deepen with continued load. Catching damage at the composite-bonding stage ($220 to $450 per tooth) is far cheaper than waiting until a crown ($1,800 to $2,500) or a root canal plus crown ($3,500+) becomes necessary. An annual photographic review tracks change and tells us when to act.
When to see a dentist sooner rather than later
Most bruxism is not urgent. The following signs justify booking sooner:
- A specific tooth that is painful when you bite or chew, especially with sharp pain on releasing pressure.
- A new chip or fracture you can feel with your tongue.
- A filling or crown that has come loose or feels different.
- Persistent jaw joint pain, locking or limited opening.
- Sudden onset of severe headaches different from your usual pattern (which warrants a GP review as well).
- Witnessed pauses in breathing during sleep, or daytime sleepiness severe enough to affect driving or work.
Frequently asked questions
How do I know if I grind my teeth at night?
The most reliable single sign is a partner reporting grinding sounds. Otherwise, look for morning jaw stiffness, headaches that fade by mid-morning, increased tooth sensitivity, and visibly flattened front teeth. A dental examination can confirm the wear pattern and rule out other causes.
Will a night guard stop the grinding or just protect the teeth?
A splint primarily protects the teeth by distributing the load and preventing enamel wear. In some patients, muscle activity also reduces over time. It is not a cure for the underlying drivers, which need separate attention.
Is teeth grinding linked to sleep apnoea?
There is a recognised association. Micro-arousals from breathing disruption appear to trigger grinding episodes. If you snore loudly, wake unrefreshed, or have witnessed pauses in breathing, raising this with your GP alongside dental treatment is worthwhile. Treating the airway sometimes reduces grinding without dental intervention.
Does Botox actually work for teeth grinding?
Botulinum toxin injected into the masseter muscles weakens the muscle and reduces grinding force for three to six months. It is generally reserved for severe cases, prominent masseter hypertrophy, or patients who have not responded to splint therapy. It complements a splint rather than replacing one.
Can stress management really help?
Yes, particularly for awake bruxism and stress-driven sleep bruxism. Cognitive behavioural therapy, mindfulness training and biofeedback have all shown reductions in clenching frequency. The effect is usually partial rather than complete, which is why most patients need a splint as well.
How much does a custom night guard cost in Sydney?
A laboratory-made hard occlusal splint typically ranges from $400 to $900, depending on design, materials and clinic. Soft or dual-laminate night guards range from $300 to $650. Private health extras commonly rebate part of the fee under ADA item 963.
Will I need to wear a splint forever?
Most patients with confirmed sleep bruxism continue to wear a splint long term, replacing it every three to five years. Some patients whose grinding was driven by a temporary stressor can wean off once the driver resolves and the wear is stable on photographic review.
About the author
Dr James Tran is the principal dentist at Lumi Dental and practises general, cosmetic and restorative dentistry in Melrose Park, Sydney. He has a particular clinical interest in conservative, evidence-based care for tooth wear, cracked teeth and jaw-related symptoms, and works closely with sleep physicians and physiotherapists when bruxism overlaps with broader sleep or musculoskeletal concerns. AHPRA registration DEN0001934469.
About Lumi Dental
Lumi Dental is a modern dental practice at Melrose Park Central, Melrose Park NSW 2114, offering general, cosmetic, orthodontic, implant, emergency and family dentistry, with sedation options available for nervous patients. The practice welcomes patients from Meadowbank, Ryde, Ermington, West Ryde, Denistone, Eastwood and the broader Sydney area.
If you suspect you grind your teeth, or your partner has mentioned it, you can book a new-patient assessment at Lumi Dental. Related reading on Lumi: night guards and occlusal splints in Sydney, cracked tooth syndrome, receding gums causes and treatment, sensitive teeth causes and treatment, and dental anxiety guide.
This article is general information only and is not a substitute for personalised dental advice. Individual diagnosis, treatment options and costs depend on your specific circumstances and should be discussed at a clinical consultation.