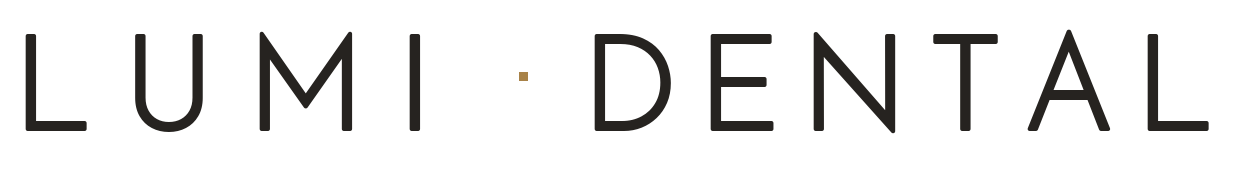About one in five Australian adults gets recurring mouth ulcers, and most people will experience at least one in their lifetime. Roughly eight in ten of those ulcers are the minor aphthous type, the small round sores you feel before you see them. Most heal on their own within ten to fourteen days, but any ulcer that lasts longer than two weeks needs a professional look, because that timeline is the single most important rule for ruling out something more serious.
Mouth ulcers are common, painful, and almost always harmless, but the way you treat them can decide whether you get back to eating and talking normally in three days or three weeks. This guide covers what causes them, what actually helps, what you can buy at a Sydney pharmacy, and the specific red flags that mean it is time to see a dentist rather than wait it out.
Key takeaways
- Most mouth ulcers heal within 10 to 14 days without treatment, but the right products can shorten that timeline and reduce pain significantly.
- The most common triggers are accidental cheek bites, sharp foods, stress, hormonal changes, and low iron, folate, or vitamin B12.
- Bonjela, SM-33, and salt water rinses are first-line options available at any Sydney pharmacy. Stronger options like Kenalog in Orabase or chlorhexidine mouthwash usually need a dentist or pharmacist consultation.
- Any ulcer that lasts longer than two weeks, bleeds spontaneously, feels numb instead of painful, or sits with a hard edge needs a clinical assessment. This rule exists to catch the rare cases that are not benign.
- If you get four or more ulcers a year, a blood test for iron, folate, vitamin B12, and coeliac antibodies often finds the trigger.
What mouth ulcers actually are
A mouth ulcer is a small open sore in the soft lining of your mouth where the protective tissue has broken down and exposed the layer underneath. The clinical name is an aphthous ulcer, and most look like a round or oval white or yellow patch with a clear red border. They typically sit on the inside of your cheeks, lips, under your tongue, on the floor of your mouth, or on the soft palate at the back. They do not usually appear on the firm, attached gum tissue or the hard palate, which is one quick way clinicians tell them apart from cold sores.
The pain is out of proportion to the size. Even a one millimetre ulcer can make eating citrus, spicy food, or anything salty deeply uncomfortable, because the exposed nerve endings are right at the surface. That intensity is normal and not a sign of anything wrong.

The three main types
Not every ulcer behaves the same way, and the type usually predicts how long you will be dealing with it.
Minor aphthous ulcers
These are the standard, garden-variety mouth ulcer that most people get. They are smaller than 5 mm across, oval, and heal in 7 to 14 days without scarring. About 80% of recurring ulcer cases are this type.
Major aphthous ulcers
Larger than 10 mm, deeper, and more painful. They can take 4 to 6 weeks to heal and sometimes leave a small scar. Major aphthous ulcers usually need stronger topical treatment from a dentist or oral medicine specialist.
Herpetiform ulcers
The name is misleading because they have nothing to do with the herpes virus. These are clusters of many tiny pinpoint ulcers that can merge into one larger irregular sore. They are less common but tend to recur and benefit from prescription treatment.
Why you keep getting them
The honest answer is that researchers still do not fully understand why some people get a few ulcers a year and others get one every month. What is clear is that ulcers are usually triggered rather than caused, and removing the trigger is the most reliable way to stop the cycle. The common triggers are listed below.
Local trauma
Accidentally biting the inside of your cheek, scratching your gum with a piece of crusty bread, an ill-fitting partial denture, or the rough edge of a fractured tooth or filling will all break the lining and seed an ulcer. About a third of all isolated ulcers can be traced to a single mechanical injury.
Stress and sleep deprivation
Stress and short sleep both suppress immune function and shift cortisol patterns. Patients commonly report a flare around exam periods, project deadlines, or after a poor week of sleep. The link is well documented but not a personal failing, it is simply how the immune system behaves under load.
Nutritional deficiencies
Low iron, low folate, and low vitamin B12 are the three classic blood-level deficiencies linked to recurrent ulcers. Vitamin D and zinc are also implicated in some studies. Australians on plant-based diets, women with heavy periods, and people with absorption problems like coeliac or Crohn's disease are the groups most likely to be deficient without realising it.
Hormonal changes
Ulcers tend to cluster around menstrual cycles, pregnancy, and perimenopause. Women report recurring ulcers about twice as often as men, which is consistent with hormonal sensitivity playing a role.
Food triggers and toothpaste
Some people genuinely react to specific foods, most often citrus, tomato, chocolate, coffee, nuts, and strong cheese. Sodium lauryl sulphate, the foaming agent in most regular toothpastes, also triggers ulcers in a minority of people. Switching to an SLS-free toothpaste for six weeks is a cheap and reasonable test if you suspect this.
Medical conditions
Recurring ulcers can occasionally be a flag for coeliac disease, inflammatory bowel disease, Behcet's syndrome, or HIV. They can also be a side effect of medications including some non-steroidal anti-inflammatories, nicorandil, and certain chemotherapy drugs. If your ulcer pattern has changed suddenly or is unusually severe, mention it to your GP.
Treatments available in Sydney
Treatment for mouth ulcers sits on a ladder. Most people only need the first two rungs. The table below covers what each option does, where to get it, and rough pricing.
| Treatment | What it does | Where to get it | Typical cost (Sydney) |
|---|---|---|---|
| Warm salt water rinse | Reduces bacterial load and inflammation. Free, gentle, and safe for any age. | Home (1 teaspoon salt in a cup of warm water, 3-4 times daily) | Free |
| Bonjela gel | Topical analgesic with mild antiseptic. Numbs the area for 1-2 hours. Not for under 16s due to choline salicylate. | Any pharmacy, supermarket, Chemist Warehouse | $8 to $12 |
| SM-33 paint | Combination liquid with lignocaine, salicylic acid, and tannins. Strong numbing effect, slightly bitter taste. | Pharmacy, sometimes pharmacist-recommended | $15 to $20 |
| Difflam (benzydamine) mouthwash or spray | Anti-inflammatory rinse, useful for ulcers in awkward spots like the back of the throat or under the tongue. | Pharmacy | $12 to $18 |
| Chlorhexidine mouthwash (Savacol, Curasept) | Antibacterial rinse that can reduce ulcer duration and prevent secondary infection. Use for no more than 10 days at a time due to temporary staining. | Pharmacy | $15 to $25 |
| Kenalog in Orabase (triamcinolone paste) | Topical corticosteroid in a sticky paste that adheres to the ulcer. Can halve healing time for painful or persistent cases. | Pharmacist-only or dentist prescription | $25 to $40 |
| Dentist assessment and prescription | For major ulcers, recurrent cases, or anything that has not healed in two weeks. May include a steroid mouthwash, biopsy, or referral. | General dentist or oral medicine specialist | $80 to $150 examination, plus any treatment |
A good practical rule is to start with salt water rinses on day one, add Bonjela or SM-33 for daytime pain relief, and add a chlorhexidine rinse once a day for the first three days if the ulcer is large or you have several at once. If you are not seeing meaningful improvement by day five, the dentist-prescribed paste shortens healing reliably for most people.
When to see a dentist
Most mouth ulcers do not need a dentist visit. The visits that do matter are the ones below.
- An ulcer that has not healed in 14 days. This is the single most important rule. Healthdirect and the Australian Dental Association both flag the two-week mark as the point where the ulcer needs a clinical assessment, regardless of how big or small it looks.
- Ulcers that bleed on their own. Ordinary mouth ulcers can sting and weep, but they do not usually bleed spontaneously when you are not eating or brushing the area.
- A painless ulcer. Standard ulcers are very painful. A sore that you only notice when you happen to look in the mirror is more concerning than a small ulcer that hurts.
- A hard edge or raised border. Run your tongue over the ulcer. The edge of a normal ulcer is soft. A firm, indurated, or rolled edge is a clinical red flag.
- Numbness in the area. Loss of sensation in the lip, tongue, or floor of the mouth alongside an ulcer is a flag.
- Frequent recurrence. Four or more ulcers per year warrants a blood test panel for iron, ferritin, folate, vitamin B12, and coeliac antibodies. This is often the moment we find a deficiency the patient did not know about.
- Ulcers that started after a new medication. Worth flagging so we can review whether the medication is the trigger.
One last point on the two-week rule. About 9 in 10 people who are diagnosed with mouth cancer at an early stage are still alive five years later. That number drops to roughly 5 in 10 when it is found late. The cost of a 20-minute dental visit to check a slow-healing ulcer is small relative to the cost of finding something three months later than you needed to.

Mouth ulcer or something else
Three conditions get confused with mouth ulcers regularly. The differences matter because the treatment is different.
Cold sores
Cold sores (herpes labialis) are caused by the herpes simplex virus and appear on the outside of the lip or at the lip border, not inside the mouth. They start as a cluster of tingling blisters that burst, crust, and scab over. Antiviral creams like aciclovir help if started early. Mouth ulcers do not respond to antivirals.
If your "ulcer" is actually a dental abscess (a painful firm swelling on the gum next to a specific tooth), that is a different problem entirely and one that gets worse if you wait. The tooth abscess guide covers the signs and the treatment pathway.
Oral thrush
Thrush is a fungal infection that shows as white patches you can wipe away with gauze, leaving a red base. It is common after a course of antibiotics, in people using steroid inhalers without rinsing, and in babies. Treatment is antifungal, not anti-inflammatory.
Traumatic ulcer from a sharp tooth or denture
If your ulcer keeps coming back in the same exact spot, the cause is almost always mechanical. A sharp edge on a back tooth, a broken filling, or a denture that has shifted will keep re-injuring the same patch of tissue. The fix is to smooth or repair the cause, not just treat the ulcer.
Preventing the next one
Prevention is more realistic for some people than others. If you have a clear trigger, removing it works. If your ulcers are idiopathic (no identifiable cause), prevention is patchier but still worth trying.
- Use an SLS-free toothpaste for six weeks. Brands available in Sydney pharmacies include Sensodyne Pronamel, Biotene, and several Grants and Jack N' Jill options. If your ulcer rate drops noticeably, you have found a trigger.
- Address any sharp edges. If a tooth or filling feels rough, get it smoothed at your next check up. A two-minute polish can stop a recurring cheek ulcer.
- Get a blood test if you are getting more than four ulcers a year. Iron, ferritin, folate, vitamin B12, and coeliac antibodies are the standard panel. Replacement therapy is usually straightforward and stops the cycle for most deficiency-driven cases.
- Eat slowly with hard foods. Crusty bread, hard pretzels, crisps, and toast are common culprits for a sudden cheek bite.
- Manage stress and sleep where you can. Easy to say, harder to do, but worth keeping in mind during high-load periods.
- Maintain your routine cleans. A clean mouth heals faster. A six-monthly hygienist visit removes the plaque and tartar that prolong inflammation around recurring ulcers.
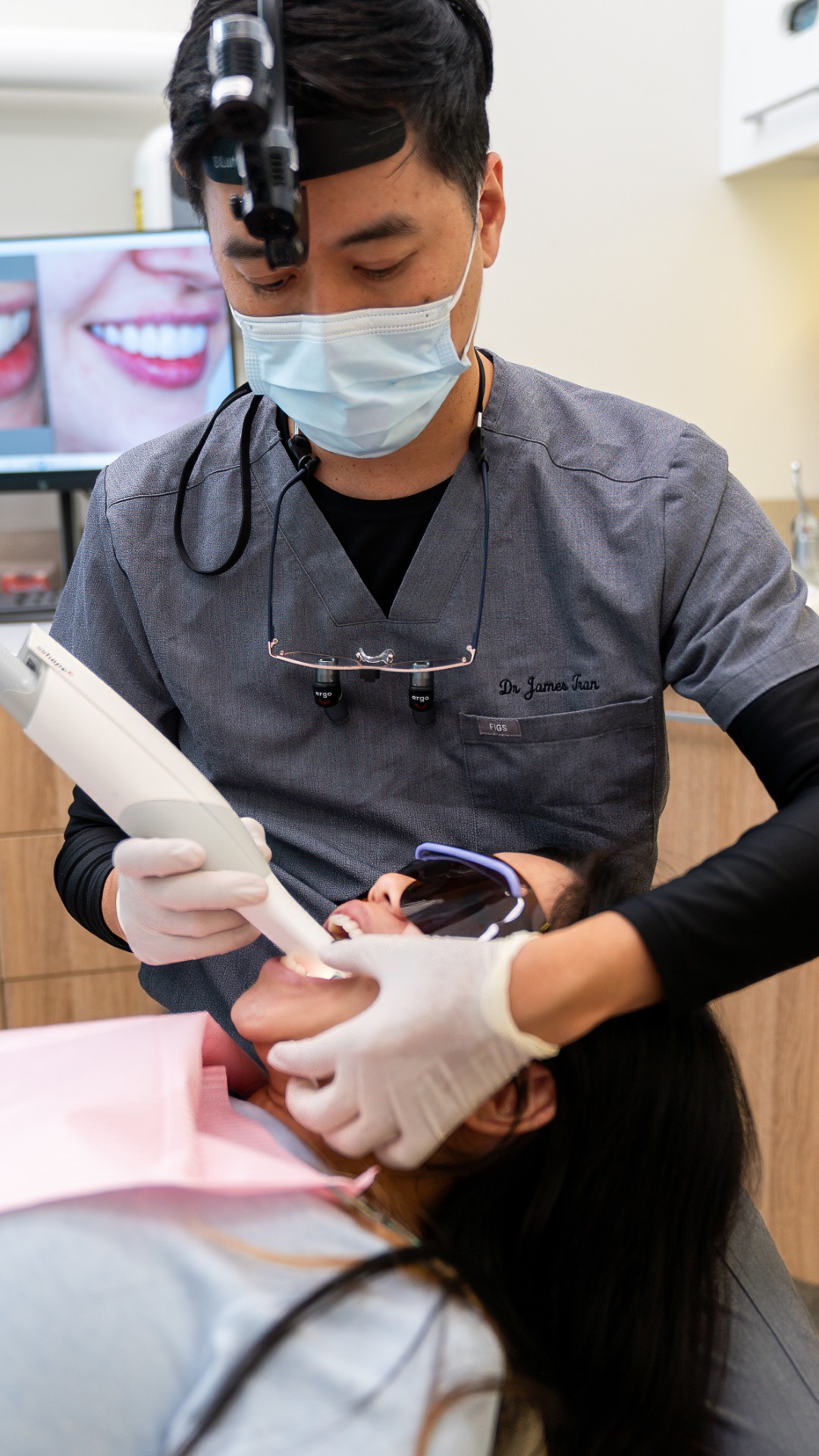
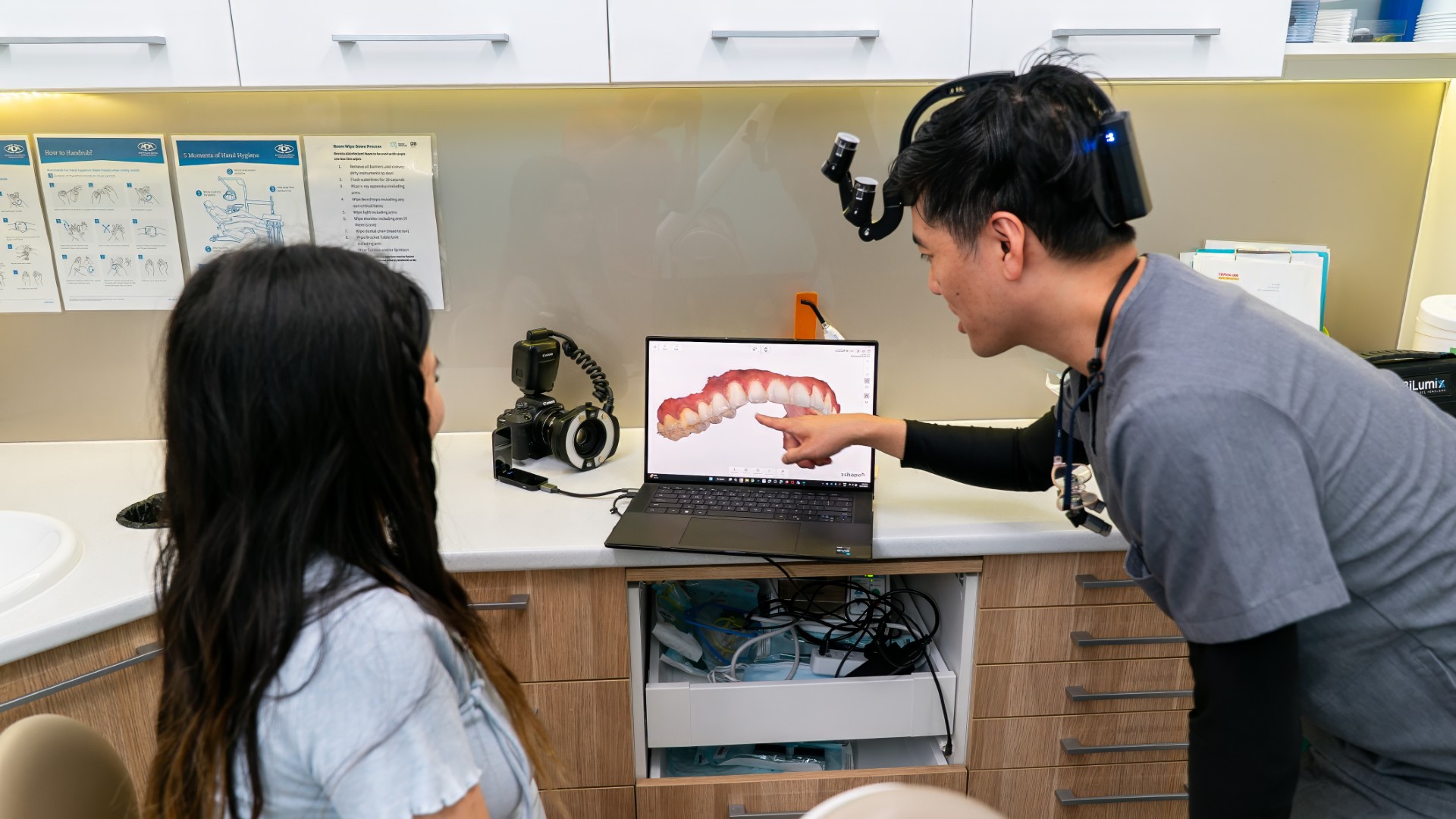
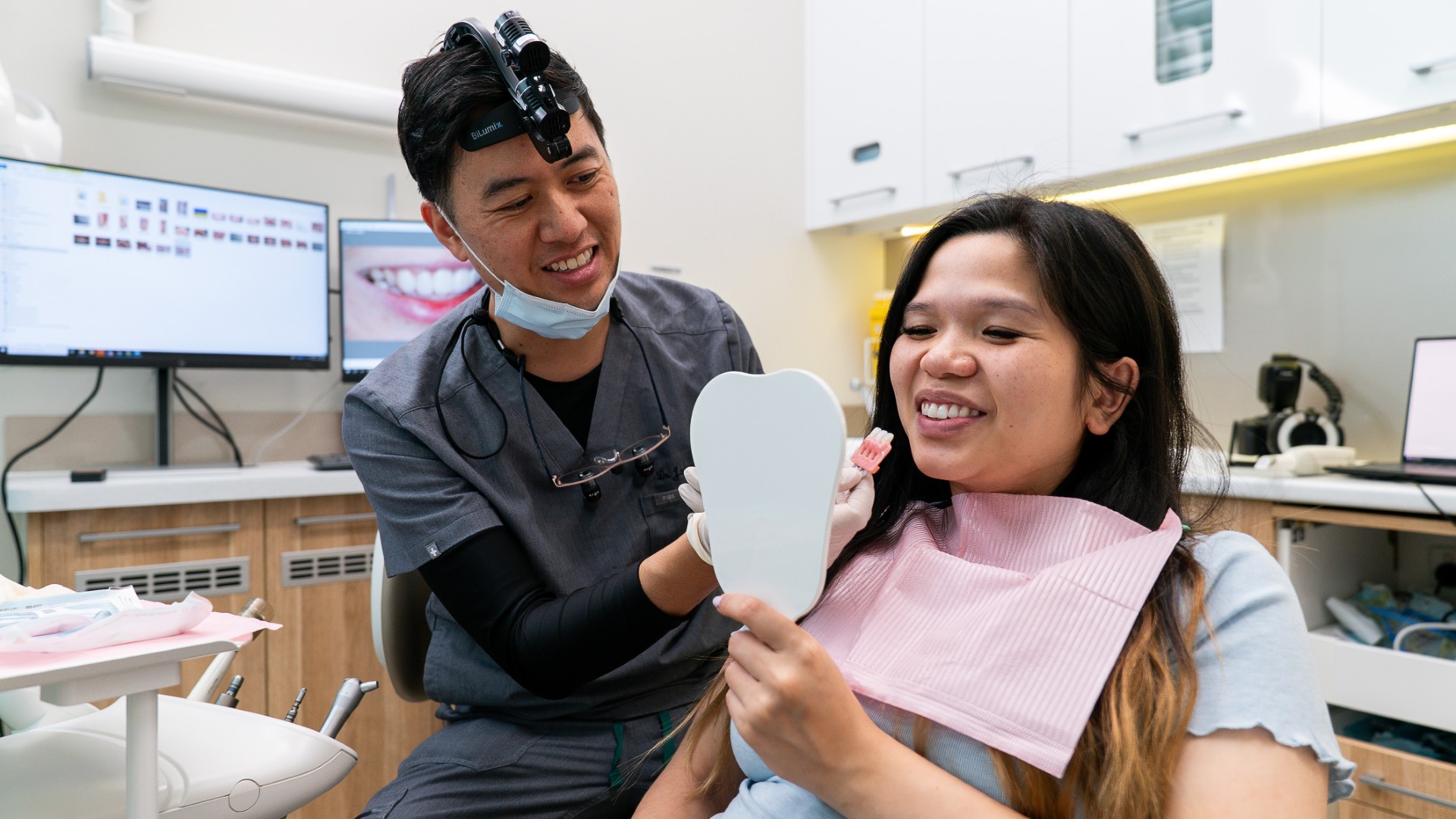
How Lumi Dental approaches mouth ulcer cases
At Lumi Dental in Melrose Park, ulcer assessments are typically part of a general check up unless you book a focused visit. We will look at the ulcer itself, examine the surrounding tissue, check for sharp edges or rough restorations that could be causing it, and palpate the floor of your mouth and neck. If the ulcer has been present for more than two weeks or has any of the red flags above, we will either prescribe a topical steroid paste, arrange a referral to an oral medicine specialist at Westmead, or order the appropriate blood tests. We do not photograph or document ulcers as before-and-after material and we will never make outcome guarantees on healing time, because the biology varies person to person.
If you want to book a focused mouth ulcer assessment, our new patient offer is the easiest entry point. A comprehensive exam covers the ulcer and a full oral cancer screening at the same time, which is the right scope for anything that has worried you for more than two weeks.
Frequently asked questions
How long should a mouth ulcer take to heal?
Minor mouth ulcers usually heal within 7 to 14 days without treatment. Larger ulcers can take up to four weeks. Anything that has not closed up by the two-week mark needs a clinical assessment, even if it is small and painless.
Are mouth ulcers contagious?
No, standard aphthous mouth ulcers are not contagious. You cannot pass them on by sharing utensils, kissing, or drinking from the same cup. The condition that often gets confused with mouth ulcers is cold sores, which are caused by the herpes simplex virus and are contagious through skin contact.
Can I get a mouth ulcer from kissing or sharing a drink?
You cannot catch a mouth ulcer from another person. You can catch the herpes simplex virus, which causes cold sores on the outside of the lip. The two are often confused. Cold sores are external, on the lip border, and start as a tingling cluster of blisters. Mouth ulcers are internal, in the soft lining, and appear as a single round white or yellow sore.
What is the fastest way to heal a mouth ulcer?
For most adults, combining a chlorhexidine mouthwash with a topical corticosteroid paste like Kenalog in Orabase produces the fastest reliable healing, typically cutting recovery time in half. The combination needs a pharmacist or dentist conversation rather than self-selection. Salt water rinses and Bonjela can keep pain manageable while the ulcer heals on its own timeline.
Why do I keep getting mouth ulcers in the same spot?
Recurring ulcers in the exact same location are almost always mechanical. A sharp tooth, fractured filling, or shifted denture is re-injuring the same patch of tissue. A dental check can usually identify the source in a few minutes, and a polish or small repair will stop the cycle.
Can children use Bonjela?
Bonjela Mouth Ulcer gel is acceptable from 4 months of age in Australia, but the children's version (Bonjela Junior) is formulated without choline salicylate, which is safer for under 16s. Read the label carefully or ask your pharmacist before using adult Bonjela on a child.
Should I worry about an ulcer on my tongue?
Ulcers on the side or underneath the tongue are common and usually heal on their own. The concern is duration, not location. Any tongue ulcer that has not healed in two weeks, or one that is hard, raised, or painless, should be seen by a dentist. The tongue is a relatively high-risk site for oral cancer compared to the cheek or lip.
Do mouth ulcers mean I have a vitamin deficiency?
Sometimes, but not always. About a quarter of patients with recurring mouth ulcers turn out to have low iron, folate, or vitamin B12. If you are getting four or more ulcers a year, ask your GP or dentist for a blood test. If the panel is normal, the cause is more likely stress, hormonal, or unidentified. Patients with recurring soft-tissue irritation sometimes also experience sensitive teeth or persistent bad breath, both of which point back to similar inflammatory and dietary triggers.
The short version
Mouth ulcers are usually harmless, almost always painful out of proportion to their size, and almost always heal in under two weeks. Salt water rinses and Bonjela handle most of them. The rule that matters most is the two-week rule. If an ulcer has stuck around longer than that, has a hard edge, bleeds on its own, or sits alongside numbness, book a check rather than wait it out. Catching the rare cases that are not benign matters far more than over-treating the common ones that are.
If you are in Ryde or Melrose Park and want a focused assessment, get in touch with Lumi Dental and we will fit you in.