Around 5,577 Australians are expected to be diagnosed with a head and neck cancer (including lip and oral cavity) in 2025, and roughly three quarters of cases occur in men. When oral cancer is found at an early, localised stage, the 5-year relative survival rate climbs to about 75%. When it is found late, survival drops sharply. The most reliable way to catch a lesion early is a quick screening at your regular dental check-up, supported by a monthly self-check at home.
This guide explains what an oral cancer screening involves in Sydney, who should be screened and how often, what your dentist looks for, how to do a 7-step self-check at home, the risk factors that matter most in Australia, and what an oral cancer screening typically costs.
Key Takeaways
- Oral cancer screening is a 2 to 5 minute visual and tactile check that fits inside a routine dental examination.
- The Australian Dental Association recommends an oral cancer screening at least once a year for every adult, including denture wearers.
- Any mouth ulcer, red patch, white patch or lump that lasts longer than 2 weeks should be reviewed by a dentist or doctor.
- Tobacco, alcohol, HPV, sun exposure to the lips and betel quid are the main modifiable risk factors in Australia.
- Most oral cancer screenings in Sydney are bundled into the periodic oral examination (ADA item 012) at no additional charge; a stand-alone screening typically costs $60 to $120.
- The 5-year survival rate is around 75% when oral cancer is caught early, compared to 30 to 40% for advanced-stage disease.
What is an oral cancer screening?
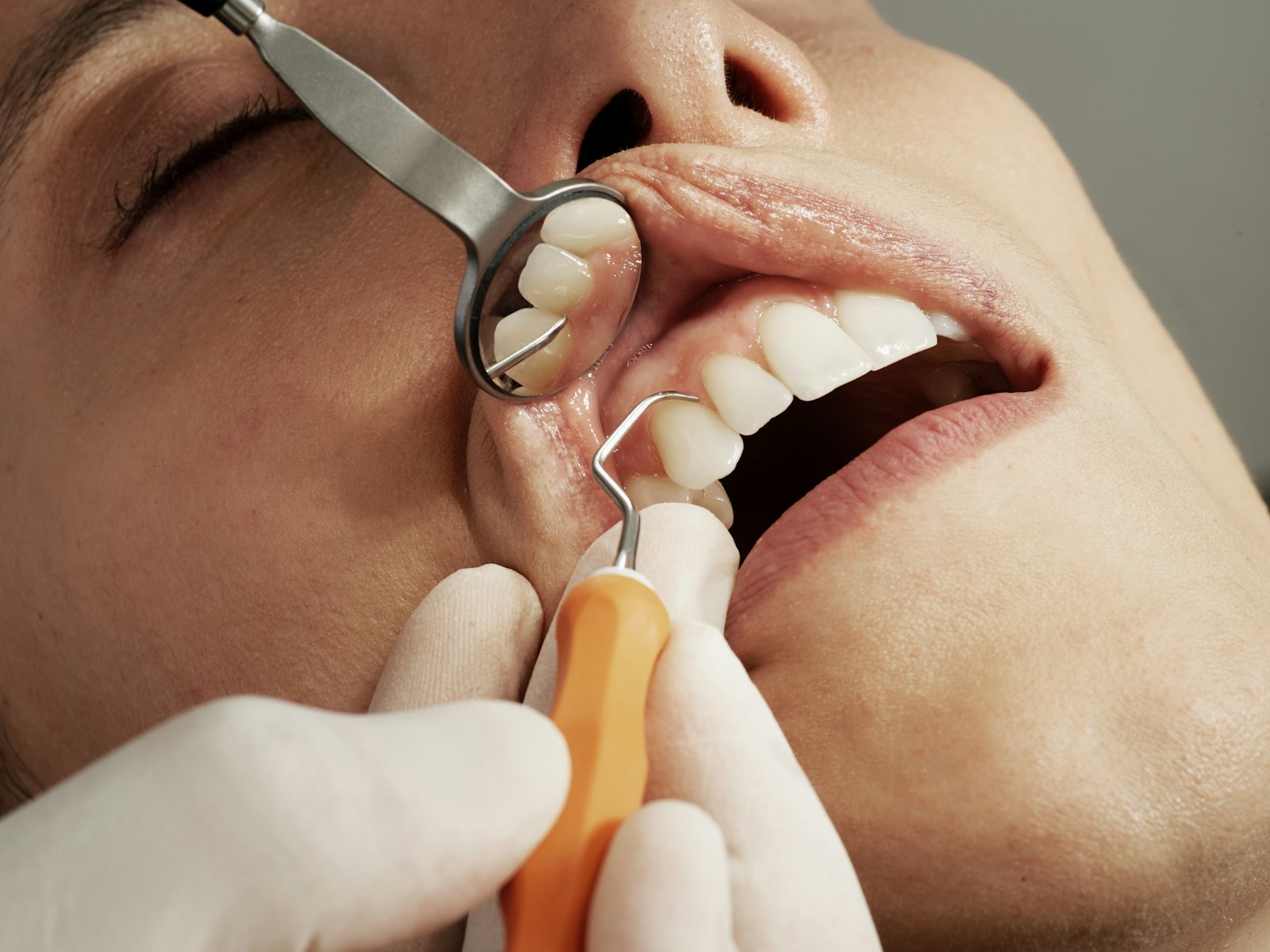
An oral cancer screening is a structured visual and tactile examination of the mouth, lips, jaw and neck looking for the early signs of cancer or pre-cancerous changes. It is not a single test or a biopsy. It is a routine check that any general dentist in Sydney can perform during a standard appointment.
During the screening, your dentist will:
- Inspect the face, lips, jawline and neck for asymmetry, lumps or skin changes.
- Palpate the lymph nodes under the jaw, along the sides of the neck and behind the ears.
- Examine the inside of the cheeks, the gums, the floor of the mouth, the roof of the mouth, the tonsillar area and the entire surface of the tongue, including the underside and lateral borders.
- Gently hold the tongue with gauze and pull it forward to view the rear lateral border and base of the tongue, where many oral cancers begin.
- Feel the floor of the mouth with two fingers (one inside, one under the chin) to detect any firmness or thickening that is not visible on inspection.
The whole process is painless and takes 2 to 5 minutes. If anything looks or feels unusual, the dentist will document the location and size of the finding, photograph it where possible, and either review it in 2 weeks or refer you for biopsy.

Who should be screened and how often?
The Australian Dental Association's policy statement on oral cancer recommends that an oral cancer screening forms part of every comprehensive dental examination and that all adults, including those who wear dentures and have no natural teeth, should be screened at least once a year.
Frequency should increase with risk. Use the table below as a general guide and discuss your personal interval with your dentist.
| Risk profile | Suggested screening interval | Why |
|---|---|---|
| Adult with no major risk factors | Every 12 months | Aligned with the ADA baseline recommendation. |
| Smoker or recent ex-smoker (within 10 years) | Every 6 months | Tobacco use roughly doubles oral cancer risk and the risk persists for years after quitting. |
| Regular drinker above the Australian alcohol guidelines | Every 6 months | Alcohol is a dose-dependent risk factor; combined with smoking the risk multiplies. |
| Previous head, neck or oral cancer | Every 3 to 6 months | Recurrence and second primary cancers are most common in the first 5 years. |
| Known HPV-positive or strong family history | Every 6 to 12 months | Persistent oral HPV infection is a recognised driver of oropharyngeal cancer. |
| Outdoor worker with significant lip sun exposure | Every 6 to 12 months | Lip cancer is closely linked to UV exposure in Australia. |
| Denture wearer with no natural teeth | Every 12 months | Cancer can develop under or around dentures; routine screening remains important. |
The 7-step home self-check
A monthly self-check takes about 5 minutes and can flag a change long before it shows up at your next dental appointment. The Australian Dental Association and Mouth Cancer Foundation both encourage a regular self-examination. Stand in front of a well-lit mirror with clean hands and follow these steps.
Step 1. Face and neck
Look at your whole face in the mirror. Note any new asymmetry, swelling or skin change. Run your fingers down the sides and front of your neck and under your jaw, feeling for any tender or firm lumps.
Step 2. Lips
Pull your upper lip up and your lower lip down. Look at the inside surface and the wet-dry border. Feel the lips between your finger and thumb, checking for any rough patch, persistent crack or hard area.
Step 3. Cheeks
Open your mouth and use your finger to pull each cheek outwards. Look for red patches, white patches, ulcers or any change in colour or texture. Gently squeeze each cheek between your finger and thumb to feel for lumps.
Step 4. Roof of the mouth
Tilt your head back and open wide. Look along the hard palate at the front and the soft palate at the back. Run a finger along the surface, feeling for any thickening or rough area.
Step 5. Tongue
Stick your tongue straight out and look at the top surface. Move it side to side and inspect the left and right edges, where many oral cancers start. Most importantly, lift the tongue to the roof of the mouth so you can see the underside and the floor of the mouth. Use a clean finger to feel for any firmness on the sides or under the tongue.
Step 6. Floor of the mouth
With the tongue lifted, look at the floor of the mouth on both sides of the frenulum (the thin band of tissue under the tongue). This area is a common hiding spot for early lesions.
Step 7. Throat and tonsils
Open wide and say "ahh". Look at the back of the throat and the tonsillar pillars on each side. Note any persistent redness, ulceration or asymmetry between the two sides.
The goal of the self-check is not to diagnose anything yourself. It is to spot a change early so you can have it looked at within 2 weeks if it does not resolve.

What to look for: the 2-week rule
Oral cancer can appear in many forms. Some lesions are obvious, but many look like a routine ulcer, a denture rub or a bitten cheek in the early stages. The rule that applies internationally and is reinforced by the Australian Dental Association is the 2-week rule: any of the following changes that have not resolved within 2 weeks deserve a review by a dentist or doctor.
- A mouth ulcer or sore that does not heal within 2 weeks, particularly if it is painless, firm at the base, or has rolled edges.
- A red patch (erythroplakia) that cannot be wiped away. Red patches carry a higher risk of being pre-cancerous or cancerous than white patches.
- A white patch (leukoplakia) that cannot be wiped away. Most are benign, but a small proportion progress to cancer.
- A mixed red and white patch (erythroleukoplakia). These carry the highest risk of dysplasia or invasive change.
- An unexplained lump, thickening or numbness in the cheek, tongue, palate, gum or neck.
- Persistent sore throat, hoarse voice or difficulty swallowing lasting more than 3 weeks.
- A loose tooth with no obvious dental cause, or dentures that suddenly stop fitting properly.
- Bleeding in the mouth that cannot be explained by gum disease, brushing or trauma.
Pain is a poor early indicator. Many oral cancers are painless until they reach an advanced stage, which is one of the reasons routine screening is so important.
Risk factors that matter in Australia
Most oral cancers are linked to modifiable lifestyle exposures. Understanding the major risk factors helps you make practical decisions and lets your dentist tailor how often you should be screened.
Tobacco
Any form of inhaled or chewed tobacco raises oral cancer risk. People who smoke are roughly twice as likely to develop oral cancer than those who do not, and the risk grows with the duration and quantity of use. Cigarettes, cigars, pipes, hand-rolled tobacco and smokeless tobacco all carry risk. Vaping is a newer exposure and the long-term oral cancer risk is still being studied, but the available evidence does not suggest it is risk-free.
Alcohol
Alcohol is a dose-dependent risk factor. Even light drinking, defined in the literature as one standard drink per day, has been associated with an increase in oral cancer risk, and heavy drinkers can be up to 6 times more likely to develop the disease. The Australian Guidelines recommend no more than 10 standard drinks per week and no more than 4 in a single day to reduce alcohol-related disease.
Tobacco and alcohol combined
The combination is the most important point. Using tobacco and alcohol together does not simply add the two risks. It multiplies them. Heavy drinkers who also smoke face a substantially higher risk than either exposure alone.
HPV
Persistent infection with human papillomavirus, especially HPV-16, is now recognised as a driver of oropharyngeal cancers affecting the base of tongue and tonsil. HPV-related cancers tend to affect a younger demographic than tobacco-related cancers and are increasing in incidence in Australia. The Gardasil 9 vaccine, offered free through the National Immunisation Program for adolescents aged 12 to 13 in Australia, protects against the HPV types most strongly linked to oropharyngeal cancer.
Sun exposure
Lip cancer is closely associated with cumulative UV exposure, which is a particular concern in the Australian climate. Outdoor workers and people who spend long hours in the sun without lip protection are at elevated risk. SPF 30 or higher lip balm, a wide-brimmed hat and shade reduce the risk meaningfully.
Betel quid
Areca nut (betel quid), often chewed in South Asian, South-East Asian and Pacific communities, is a powerful oral carcinogen. It can cause oral cancer on its own and the risk is amplified when chewed with tobacco. Sydney's diverse demographics make this an important risk factor to ask about in any thorough screening.
Other factors
Older age (most cases occur after 40), male sex, family history of head and neck cancer, long-term immunosuppression (such as after an organ transplant), poor diet low in fresh fruit and vegetables, and chronic irritation from sharp teeth or poorly fitting dentures can all contribute.
What to expect at a Lumi Dental screening
At Lumi Dental in Melrose Park, an oral cancer screening is built into every comprehensive examination at no additional cost. The process is straightforward.
- Health history. We ask about smoking, alcohol, betel quid, sun exposure, HPV history, family history and any new lumps, ulcers or symptoms.
- Extra-oral examination. Dr James Tran examines the face, lips and neck and palpates the lymph nodes.
- Intra-oral examination. Every surface of the mouth is inspected and palpated using a structured sequence so nothing is missed. The tongue is held with gauze so the lateral and rear borders can be properly viewed.
- Documentation. Anything unusual is recorded with a clinical note, a photograph and a measurement so we can compare at the next visit.
- Plan. If a lesion is suspicious, we explain the next step clearly. Most lesions are reviewed in 2 weeks. If a biopsy or specialist referral is needed, we arrange it with an oral medicine specialist or oral and maxillofacial surgeon in the Ryde and Macquarie Park area.
Oral cancer screening cost in Sydney
For most patients in Sydney, an oral cancer screening is included in the periodic or comprehensive oral examination at no extra charge. A stand-alone or adjunctive screening may be billed separately if it involves additional time or technology. The table below shows typical Sydney private fees alongside the relevant Australian Dental Association (ADA) item codes.
| Service | ADA item code | Typical Sydney fee | What is included |
|---|---|---|---|
| Periodic oral examination with screening | 012 | $70 to $110 | Standard 6-monthly check; oral cancer screening included. |
| Comprehensive oral examination with screening | 011 | $95 to $160 | New patient or first detailed exam; full intra and extra-oral cancer screening included. |
| Limited oral examination (new lump or lesion) | 013 | $60 to $100 | Focused examination of a specific concern such as a new ulcer or lump. |
| Consultation (extended examination) | 014 | $95 to $130 | Longer appointment for complex history or multiple concerns. |
| Stand-alone adjunctive screening (fluorescence, dye, etc.) | Practice-dependent | $40 to $90 | Optional fluorescence light or toluidine blue dye check. Use is not universal and the ADA notes evidence for routine adjunctive technology is still evolving. |
| Biopsy (if needed) | 165 or 311 series | $200 to $600 | Removal of tissue for laboratory diagnosis. Item code depends on size and location. |
If you hold private health insurance with extras cover, the periodic and comprehensive examinations (items 011 and 012) are usually covered in full or close to it on most policies. The Child Dental Benefits Schedule covers eligible children up to age 17 and includes the same examination items.
When you should not wait
Some symptoms warrant an urgent appointment rather than waiting for your next routine check. Contact your dentist or doctor promptly if you notice any of the following.
- A mouth ulcer or sore that has not started to heal after 2 weeks, especially if painless.
- A red, white or mixed patch in the mouth that you can see has been there for more than 2 weeks.
- A lump, thickening or area of numbness in the cheek, tongue, lip or neck.
- A persistent hoarse voice or change in voice quality lasting more than 3 weeks.
- Difficulty swallowing or a feeling of something caught in the throat.
- A loose tooth without a dental cause, or dentures that suddenly do not fit.
- Unexplained bleeding from the mouth or a sore that bleeds easily on contact.
- A non-healing crusty or scaly patch on the lip.
None of these symptoms confirm cancer. Most turn out to be benign. The point is that catching the small number that are cancerous at an early stage makes a major difference to outcomes.
How Lumi approaches oral cancer screening
Every adult who books a check-up at Lumi Dental receives a structured oral cancer screening as part of the appointment. Dr James Tran follows a standard intra-oral and extra-oral protocol so the same areas are examined at every visit and any change between visits can be detected. Where the screening identifies a finding that warrants further investigation, we explain the options clearly, take photographs for monitoring and arrange specialist referral where appropriate. We do not use a single screening tool as a substitute for clinical judgement, and we do not charge separately for the cancer screening component of a routine examination.
Frequently asked questions
How often should I have an oral cancer screening in Sydney?
The Australian Dental Association recommends at least once a year for every adult, including denture wearers. If you smoke, drink regularly, have a history of HPV, work outdoors with significant lip sun exposure or have a personal or family history of head and neck cancer, every 6 months is more appropriate. Your dentist can recommend an interval based on your individual risk profile.
Does an oral cancer screening hurt?
No. The screening is a visual inspection combined with gentle palpation of the lymph nodes, cheeks, tongue and floor of the mouth. The tongue is held briefly with gauze to allow a proper view of the lateral and rear borders. There are no injections, no scrapings and no instruments other than a mirror and a gloved hand. The whole process takes 2 to 5 minutes.
Is oral cancer screening covered by private health insurance?
The screening is bundled into the periodic oral examination (item 012) or comprehensive examination (item 011), both of which are usually well covered by extras policies. Most patients with mid-tier or higher extras cover pay little or nothing out of pocket for a routine 6-monthly check that includes the screening. Stand-alone adjunctive screening tools may not be covered; check with your insurer in advance.
What does early-stage oral cancer look like?
Early-stage oral cancer can look surprisingly subtle. The most common appearances are a flat red patch, a thickened white patch, a mixed red and white area, or an ulcer with slightly raised, firm edges that has not healed in 2 weeks. Lesions can be painless in the early stages, which is why a regular visual check by a dentist is so important.
Can a non-smoker who does not drink get oral cancer?
Yes. While tobacco and alcohol are the most important risk factors in Australia, oral and oropharyngeal cancers also occur in people with no traditional risk factors. HPV-related oropharyngeal cancer, in particular, can affect non-smokers who do not drink heavily. Lip cancer linked to sun exposure is another route. Screening remains worthwhile regardless of lifestyle.
Is the VELscope or fluorescence light worth paying for?
Adjunctive tools such as fluorescence-based devices (VELscope, OralID), toluidine blue dye and brush biopsy kits can highlight tissue changes that are harder to see with the naked eye. The current evidence base, including the Australian Dental Association's position, is that these tools may be useful in higher-risk patients but do not replace a thorough conventional visual and tactile examination. They are optional rather than required. A skilled clinical examination remains the foundation of oral cancer screening.
What is the survival rate for oral cancer in Australia?
Australian Institute of Health and Welfare data shows that the 5-year relative survival rate for head and neck cancer (including lip) has risen from 62% in 1987 to 1991 to about 72% in 2017 to 2021. For oral cancers specifically, 5-year relative survival is around 75% when averaged across all stages, and substantially higher when caught at an early, localised stage. Survival drops sharply for advanced-stage disease, which is why early detection is the single biggest lever we have.
I had a mouth ulcer for 3 weeks. Should I be worried?
A mouth ulcer that has not healed within 2 to 3 weeks should be checked, regardless of how it looks or feels. The vast majority turn out to be benign, but the 2-week rule exists because the small minority that are not benign do much better when reviewed early. Book a focused examination (item 013) rather than waiting for your next routine appointment.
Does Lumi Dental do oral cancer screenings?
Yes. Every adult check-up at Lumi Dental in Melrose Park includes a structured intra-oral and extra-oral cancer screening as part of the periodic or comprehensive examination, at no additional charge. If you have a new ulcer, lump or patch you would like reviewed sooner, we offer focused examinations (item 013) and can usually see you within a few days.
Looking after your mouth between screenings
The most useful things you can do between dental visits are practical and modest in scope. Reduce or stop smoking and vaping. Keep alcohol within Australian guidelines. Use SPF 30 or higher lip balm when outdoors. Eat a diet rich in fresh fruit and vegetables. Make sure adolescents in your family receive the HPV vaccine through the National Immunisation Program. And once a month, in front of a mirror, run through the 7-step self-check above so you spot any change early.
If you would like a thorough oral cancer screening as part of your next dental check-up in Sydney, you can book online with Lumi Dental or read about our new patient offer. We are also happy to take a focused look at any specific ulcer, patch or lump that has been on your mind for more than a couple of weeks.
This article is general information and does not replace individual advice from a registered dental or medical practitioner. If you have a specific concern, please book an appointment so a clinician can examine you in person.
For related reading, see our guides on mouth ulcers, bad breath, gum disease, dental cleaning costs and what to do in a dental emergency.